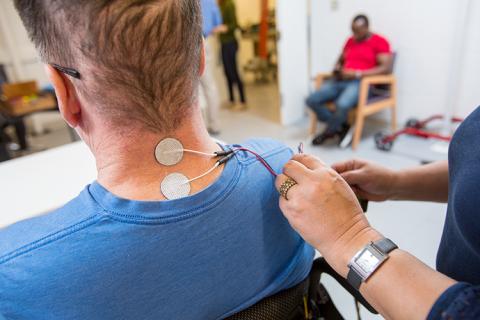
Jessica Owen is a participant in one of the Center for Neurotechnology’s transcutaneous spinal stimulation studies, which is groundbreaking research aimed at noninvasively improving upper body function for people with spinal cord injury. Owen has discovered that gradual functional improvements she gained through her participation in the study have added up to a big difference in her quality of life, leading to increased independence.
It was the middle of winter, four days before Christmas in 2012. Jessica Owen, an elementary school teacher who was then 27, and her parents, brother, sister and brother-in-law all piled into an SUV, setting out for what they thought would be a quick family vacation in Leavenworth, Washington. Although the road they took was open and clear, the trees were heavily snow-laden, and unbeknownst to the family, unusually so. As they drove over the crest of a mountain, just beyond Stevens Pass, a huge tree near the road toppled from the heavy weight of icy snow on its branches. When the tree fell, it fell hard, smashing squarely onto their car.
Only Owen’s brother escaped serious injury, managing to climb out the back window of their crumpled vehicle after the impact. Owen’s parents passed away instantly, her sister and brother-in-law both had shattered femurs, and Owen herself experienced a spinal cord injury that left her unable to feel her arms and legs. In an instant, her life was forever changed.
Owen’s injury left her with central spinal cord syndrome, which is characterized by loss of motion and sensation mainly in the arms and hands.
“I spent about four months at Harborview. After about two weeks in the intensive care unit, I was able to move to rehab and completed rehab,” said Owen, now 33. “After four months, I still could not use my hands at all. I used a wheelchair, but with a chin-drive. After that, I had to go to a skilled-nursing facility in the area, because I still had a lot of broken bones and other things to heal-up before I was ready to try to figure out how to go on.”
Owen’s injury left her with central spinal cord syndrome, which is characterized by loss of motion and sensation mainly in the arms and hands. In central spinal cord syndrome, the interior of the spinal cord has been more severely injured than its outer layers, which have been left more or less intact. Most motor control for the upper body is located in the interior of the spinal cord within the neck, while motor control for the lower body runs along the exterior of the spinal cord. Because of this anatomical feature, Owen’s lower body and legs were still impaired, but they functioned better than her upper body, arms and hands.
The injury was severe, but Owen was determined. She began going to Pushing Boundaries, an exercise-based therapy center in Redmond, Washington. She spent two years there, working out three to four days a week to regain every bit of bodily function that she could. Although she still used a wheelchair for most of the day, after two years of hard work she built-up enough strength to be able to walk short distances with crutches and transfer her body from the wheelchair into another seat (like a couch or chair) by herself.
Two years after her accident, Owen focused on going back to work. She began teaching fourth and fifth grade math for short amounts of time and over the next three years taught for longer sessions as her strength slowly increased. Eventually, she built the capacity to teach part-time and regularly substitute for her colleagues at school.
At five years after the accident, she had made remarkable progress and reclaimed her life in significant ways such as traveling more, adopting a dog and living more independently, but she realized that she was coming up against a wall.
“I still haven’t gone back to teaching full time. Part of the reason for that is my hand function,” Owen said. “I have a lot of difficulty writing, and there’s so much paper in school that even turning pages, sorting through papers and grading work is super-challenging function-wise.”
After hearing Center for Neurotechnology (CNT) Co-Director, Chet Moritz, Ph.D., speak at a Northwest Regional Spinal Cord Injury System forum about the CNT’s ground-breaking work restoring upper body function, Owen thought she might be a good candidate for an upcoming study. She approached Moritz after the talk and volunteered. After screening to confirm she was indeed a good fit, Owen was accepted as a research participant. In June 2018, she began taking part in an eight-month study with Dr. Fatma Inanici, a physician, fifth-year doctoral student in the University of Washington’s (UW’s) Rehabilitation Science program and a graduate fellow at the CNT.
Reaching beyond the wall
Dr. Inanici had been a practicing physician and faculty member at Hacettepe University Medical School in Turkey for over 20 years prior to coming to the UW to study rehabilitation science. As a physiatrist, she witnessed first-hand the limits of care for her patients with neurological conditions such as spinal cord injury, and she wanted to do more for them.
“Rehabilitation interventions typically aim to prevent secondary complications and maximize the residual function of the spinal cord. We help our patients, but especially with neurological diseases, we have a limit we cannot go beyond. Reversing the paralysis is not possible with the current standard care. That was the reason I was motivated to focus solely on research and pursue my Ph.D. education,” Dr. Inanici said. “I want to use my clinical experience to push forward the treatment options and open new avenues, if I can. I am lucky and privileged to be part of the CNT, where we work in an interdisciplinary research environment.”
During this treatment, we are improving their voluntary control of hand and arm movement. All of my participants say that even a 10 percent increase in function is making an enormous difference in their lives. For example, Jessica told me a couple days ago that for the first time she was able to button her own shirt. This is a big deal.
- CNT Graduate Fellow, Dr. Fatma Inanici
Dr. Inanici, working under Moritz’ supervision, aims to restore hand and arm function in people like Owen who have a spinal cord injury by using a new, non-invasive technique called “transcutaneous spinal stimulation,” paired with physical therapy focused on improving motor skills. “Transcutaneous” means that therapeutic electrical stimulation designed to restore neural activity in the spinal cord is applied on the surface of the skin, over the injured area.
A ground-breaking aspect of Inanici’s research is that this unique pairing of non-invasive stimulation of the spinal cord plus intensive exercise therapy increases the receptivity of spinal neurons to commands from the brain to move. This helps to “re-wire and re-organize” the body’s neural structures in ways that establish long-term improvements in hand and arm function. Although some of these functional improvements in pinch-force, grasp-strength and dexterity can seem gradual if observed in isolation, taken together, they can make a big difference in a patient’s everyday life.
“We do most of our daily activities using our hands and arms. People with paralyzed hands and arms have marked limitations in the ability of performing activities of daily living and become dependent on a caregiver, completely or partially,” Dr. Inanici explained. “Upper limb dysfunction severely restricts participation in socioeconomic activities, self-confidence and quality of life. For that reason, restoration of hand and arm function has a huge impact in everyday life.”
Over the eight months Owen participates in the study, she spends two hours, three to four times a week in the UW AMP Lab. On a typical day, Dr. Inanici applies a couple of electrodes, taped to the back of Owen’s neck, to connect her to a transcutaneous spinal stimulation machine designed by the CNT’s industry affiliate, NeuroRecovery Technologies. Dr. Inanici then leads Owen through a number of physical exercises and activities designed to strengthen muscles and improve fine motor skills.
“During this treatment, we are improving their voluntary control of hand and arm movement. All of my participants say that even a 10 percent increase in function is making an enormous difference in their lives. For example, Jessica told me a couple days ago that for the first time she was able to button her own shirt. This is a big deal.”
Gradual improvements add up to an enhanced quality of life
Owen started the study living in a house with a friend and roommate. Since then, she’s moved out and is living on her own in a new home with her dog, Odie. She has noticed significant improvements in her ability to do a wide range of everyday activities, including using buttons, zippers, taking a jacket off, putting shoes on, tying knots, opening Ziploc® bags, using a knife to cut food or open a package, no longer needing a straw for drinks, and cooking for herself. The cumulative impact of these gradual improvements means that she has been able to reduce the number of hours (and therefore the cost) of her part-time caregiver. Owen also attributes some of the inner confidence she has gained recently in regard to living independently to strength and functional improvements she is seeing as a result of this research study.
On a personal level, it’s nice just to have an easier time going through life, especially while living independently...but I'm also really hopeful that this study will be a stepping stone to the next thing that will help spinal cord injury patients.
- CNT research study participant, Jessica Owen
“I’m not all the way done with the study, and I wouldn’t say that any change has been overnight, but I would say every week, at least for the past four weeks, I can come in and say, ‘I tried this today, and I can now do this,’” Owen explained. “For example, I came in yesterday and said, ‘I did the buttons on my shirt,’ and ‘I opened the Costco [large] jar of peanut butter,’ which are things that are small, but I never did before. I am seeing a difference in just daily living and it’s making my life so much easier. I’m able to take care of myself and do everyday things, like the laundry and the dishes.”
Although the gains Owen has experienced are notable and making real impacts in her life, more study is needed to fully confirm the effectiveness of this new therapeutic approach to spinal cord injury.
“Currently, this is an experimental research study for exploring therapeutic potential of electrical spinal cord stimulation on restoration of upper limb function. Results from our first participants are quite promising. Our next steps will be to study a larger population to show the effectiveness of non-invasive spinal cord stimulation under real-world conditions,” Dr. Inanici said. “Additionally, understanding the mechanism of the beneficial effect and identifying the factors that may contribute to outcomes will guide us to optimize the treatment for an extensive range of impairments caused by spinal cord injury. So, studying a large population and continuing to collect data is important.”
Like Dr. Inanici, Owen is pleased at the restoration of her hand and arm function that the study has made possible, and she’s hopeful this research will help others as well.
“On a personal level, it’s nice just to have an easier time going through life, especially while living independently. Shaving minutes off doing the laundry, being able to button my shirt, things like that have been great, but I’m also really hopeful that this study will be a stepping stone to the next thing that will help spinal cord injury patients,” Owen said. “Hopefully, in 10 or 20 years if someone sustains a spinal cord injury, maybe it won’t even be a big deal. We just need to continue to study it and for people to show up and participate, so we can learn.”